Introduction
Meniscus tears are among the most common knee injuries. Athletes sustaining injuries during contact sports is a common mode of injury, however it is also seen during road traffic injuries, middle aged women developing meniscus root tears during house hold activities, spontaneous degenerative meniscus tears in elderly are the other causes.
Anatomy and function
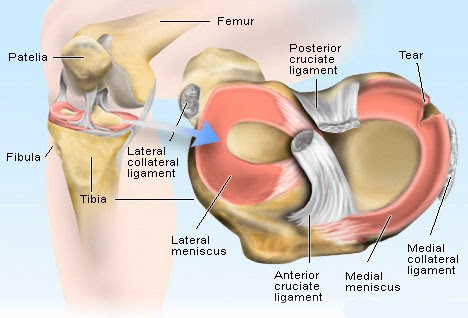
Meniscus is the rubbery tissue which cushions the knee joint, help in even distribution of joint reaction force thus reducing the chances of early wear and tear of the cartilage of the knee.
Pattern of meniscus tears
Menisci tear in different ways. Tears are noted by how they look, as well as where the tear occurs in the meniscus [anatomical location]. Common tears include bucket handle, flap, and radial/transverse tears.

Causes
Sports-related meniscus tears often occur along with other knee injuries, such as anterior cruciate ligament tears/posterior cruciate ligament tears.
Sudden meniscus tears often happen during sports. Players may squat and twist the knee, causing a tear. Direct contact, like a tackle, is sometimes involved.
Older people are more likely to have degenerative meniscus tears. Cartilage weakens and wears thin over time. Aged, worn tissue is more prone to tears. Just an awkward twist when getting up from a chair may be enough to cause a tear, if the menisci have weakened with age.
Symptoms
The most common symptoms of meniscus tear are:
- Pain
- Stiffness and swelling
- Catching or locking of your knee
- The sensation of your knee “giving way”
- You are not able to move your knee through its full range of motion
Without treatment, a piece of meniscus may come loose and drift into the joint. This can cause your knee to slip, pop, or lock.
Diagnosis
Physical examination – MacMurray’s and local tenderness along with tests for stability.
X-rays, although x-rays do not show meniscus tears, they may show other causes of knee pain, such as osteoarthritis.
Magnetic resonance imaging (MRI). This study can create better images of the soft tissues of your knee joint, like a meniscus.
Treatment
Management of meniscus tear will depend on the
- type of tear, its size, and location
- age of the patient
- activity levels of the patient
- associated ligament injuries
- pre-existing arthritis
The outside one-third of the meniscus has a rich blood supply. A minor tear in this “red” zone may heal on its own, or can often be repaired with surgery. A longitudinal tear is an example of this kind of tear.
In contrast, the inner two-thirds of the meniscus lacks a blood supply. Without nutrients from blood, tears in this “white” zone cannot heal. These complex tears are often in thin, worn cartilage. Because the pieces cannot grow back together, tears in this zone are usually surgically trimmed away.

Nonsurgical Treatment
If your tear is small and on the outer edge of the meniscus, it may not require surgical repair. As long as your symptoms do not persist and your knee is stable, nonsurgical treatment may be all you need.
However, second look MRI in 4 months’ time is always safer to confirm the healing of the meniscus tear, before declaring the patient is fit to play.
Surgical Treatment
If your symptoms persist with nonsurgical treatment, your doctor may suggest arthroscopic surgery.
Meniscus repair
Knee arthroscopy or key hole surgery is performed to identify the meniscus tear pattern, anatomic location and viability of the meniscus tissue for repair. In most of the situation’s priority will be given for meniscus repair to prevent future arthritis of knee joint.
Meniscus repair is performed
Either by/or combination of the following
all inside meniscus repair devices
inside-out meniscus repair needles and sutures
outside in meniscus repair needles and sutures
along with this certain bio stimulation procedures will be added to enhance the healing.
Partial meniscectomy
It is indicated when meniscus tear doesn’t fulfil the criteria for repair, or in degenerative tears
In this procedure, the damaged meniscus tissue is trimmed away.
Rehabilitation time for a meniscus repair is about 3 months. A meniscectomy requires less time for healing — approximately 3 to 4 weeks
With proper diagnosis, treatment, and rehabilitation, patients often return to their pre-injury abilities.




Follow us